Your Imaging. Your Choice.
General Imaging
Discover Windsong Radiology
Many patients don’t realize they have a choice when it comes to diagnostic imaging services. Windsong Radiology stands apart in offering expert, compassionate care and advanced technology to provide the answers you need. Choose you. Choose Windsong for your imaging needs.
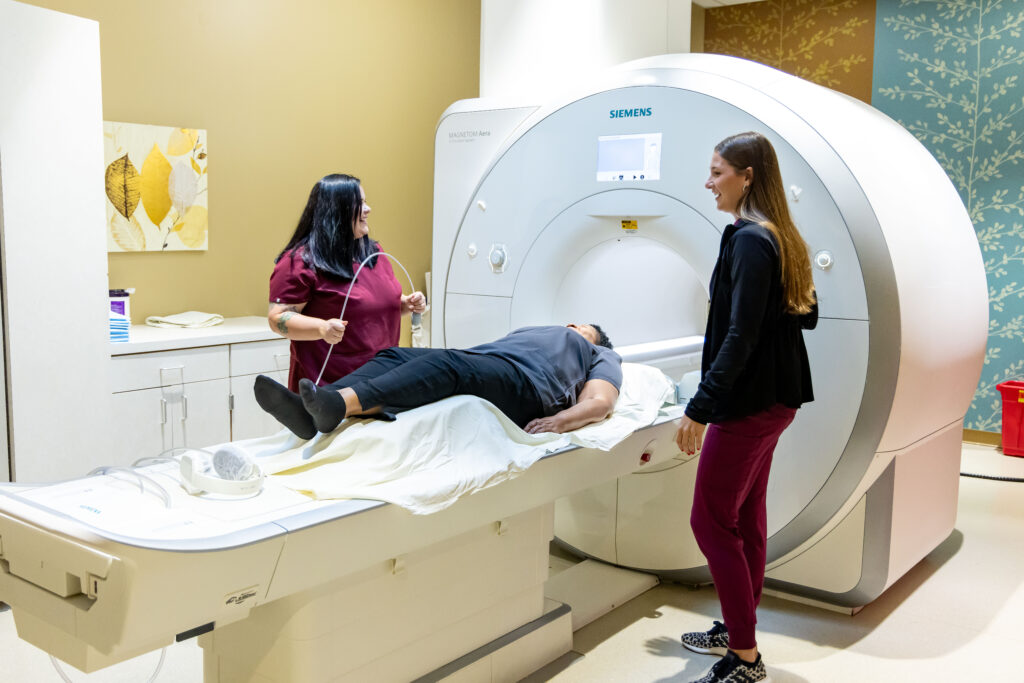
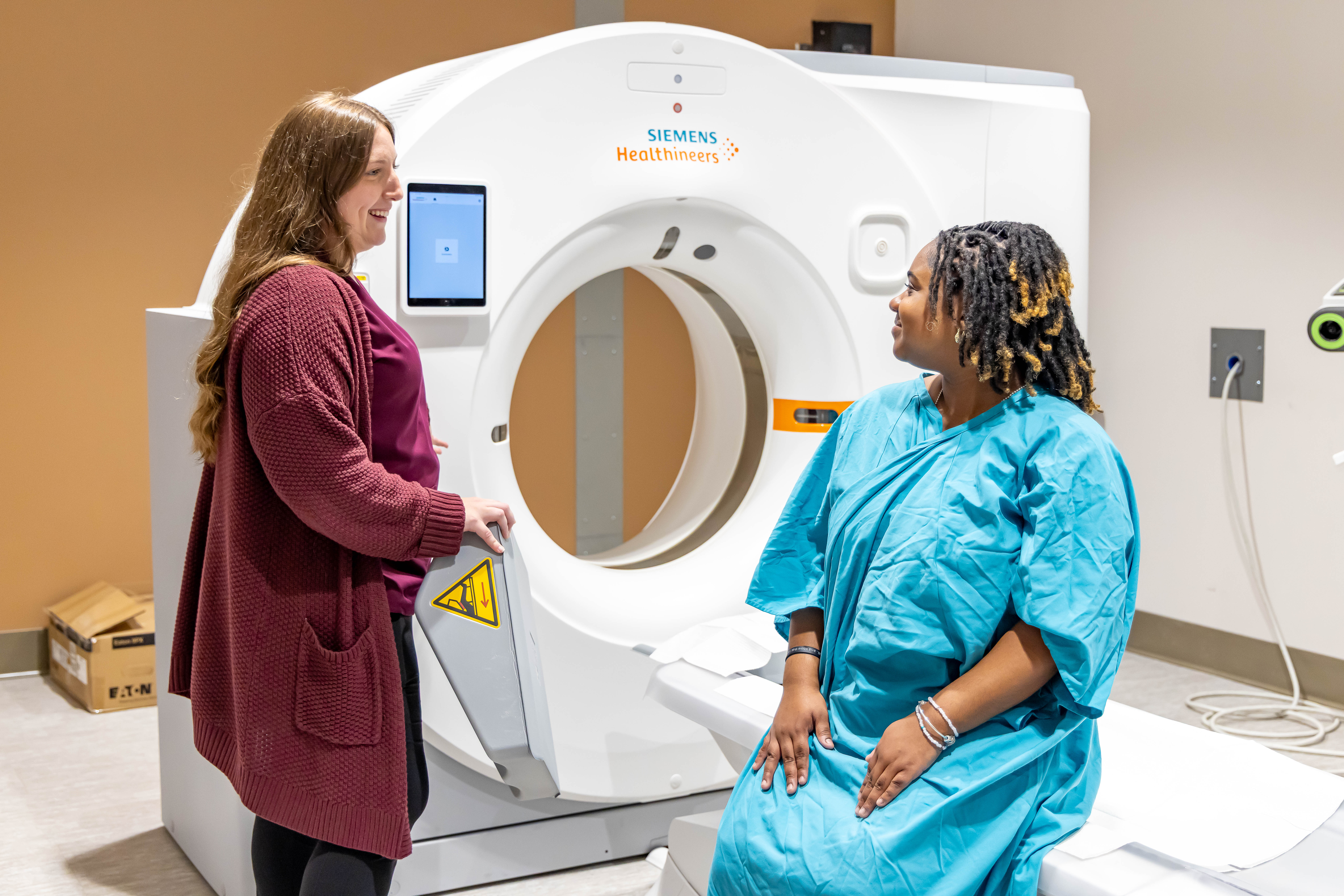
Imaging and Procedures
Medical imaging to inform accurate diagnosis can make a big difference in a patient’s treatment plan and prognosis. Windsong utilizes advanced technology and employs a team of highly trained, certified technologists to ensure a quality scan and positive patient experience. All imaging studies are interpreted by our fellowship-trained, board-certified radiologists who represent all subspecialties.

Our Physicians
Windsong’s physicians are board-certified and subspecialized, making them true experts in their fields of study – able to catch subtle differences that others may miss.